September 20, 2020
False Claim #4: “No one really knows the best way to deal with the pandemic”
As we discussed in False Claim #3, epidemiologists worldwide have been studying past pandemics and modeling community spread of highly transmissive viruses for decades. Those studies have produced clear scientific guidelines for best practices to minimize the impact of a global pandemic even, as with COVID-19, when there is no pre-existing immunity or vaccines or therapies, and the variability in detailed physiological effects of the disease is not yet understood completely. Countries that have had the best success in managing COVID-19 took the following actions: they paid close attention to these scientific guidelines; they learned from their own experiences with other recent pandemics (SARS, MERS, Ebola, H1N1 flu); they acted early and aggressively to control the spread; they provided their citizens with frequent, coherent messaging led by medical professionals; they also provided ample government aid to help citizens in weathering economic impacts; and they avoided politicizing the response to the pandemic. The U.S. is not one of those countries.

Eurasia Group, a political-risk consultancy, has analyzed the responses of worldwide governments and citizens to the COVID-19 pandemic, and highlighted the best global responses in a Time Magazine article in June 2020. The cumulative COVID-19 death rate per capita in the U.S. is compared to that in these best-practices countries, and to the world average, in Fig. 4.1. The death rates vary over an enormous range. U.S. confirmed deaths per capita are nearly 2000 times higher than those in Taiwan, more than 100 times higher than those in New Zealand and Singapore, 5 times higher than the world average and those in Germany, and more than twice as high as that in our neighbor Canada. Countries that have successfully contained the virus can be discerned in the figure because their death rates have approached a constant value, i.e., a horizontal line. The U.S. rate has never approached a horizontal line because the U.S. response has consistently failed to contain the virus, and the U.S. death rate has in fact increased in slope over the month of August. Even the successful countries may experience, and have to control, a second wave of the pandemic, as appears to be under way now in Australia.
The national differences in Fig. 4.1 do not reflect differences in luck, but rather in government policy and actions. We can learn about the best way to handle the pandemic by studying the best practices in countries that have handled it well. The single most effective approach involves an early, aggressive commitment to widespread testing, contact tracing, and seriously quarantining infected individuals while they are still few in number. For example, shortly after the first cases were recorded, the government of Taiwan quickly closed its borders, banned exports of surgical masks so they would be available to their health care professionals and their citizens, and engaged in extensive “contact tracing and mobile Sim-tracking to identify and ensure those in quarantine were actually abiding by the rules…medical officials held briefings for the public daily, and businesses were kept open by using aggressive precautionary measures like taking temperatures and providing sanitizer before patrons could enter business establishments.” Despite its proximity to mainland China, and without shuttering its economy, Taiwan has managed to keep its COVID-19 death rate below 0.3 per million inhabitants. Its great success has allowed Taiwan to produce and export critical medical supplies to other countries. Their success is certainly due, in part, to the fact that the Vice President of Taiwan is himself an epidemiologist.
Other countries that used similar techniques to succeed in limiting the spread of the disease and the extent of economic shutdowns include South Korea, Singapore and Iceland. Iceland, for example, instituted a broad and free testing program – with the highest per capita testing rate in the world – right after their first detected cases in early March 2020. South Korea similarly initiated an extensive testing program early on, and have been successful enough in tracking and isolating patients to have kept their cumulative COVID-19 death rate to 6 per million inhabitants, and have done so without shuttering much of their business community. It has helped to have a nationalized health system and a “citizenry willing to make the tradeoffs in privacy that come with deploying technologies like real-time tracking of COVID-19 patients for the sake of public health.” And despite an outbreak in overcrowded migrant housing, Singapore has kept its death rate even lower than South Korea’s.
If testing, tracking and isolation of patients are not ramped up sufficiently rapidly in a country, then it becomes necessary to institute some degree of lockdown to enforce social distancing. Simulations of community spread of infectious diseases, informed by data from earlier pandemics, have highlighted the effectiveness of early closure of schools, banning of large gatherings, and stay-at-home orders in limiting pandemic impacts. A minimal goal of such lockdowns is to slow the spread of the virus sufficiently – to “flatten the curve” – so that health care and hospital services in the country do not get overwhelmed by surges in infected patients. Community spread of the virus can be further limited by individual actions, such as wearing masks, maintaining safe distances from others in public places, and frequent hand-washing.
New Zealand has largely succeeded by following this approach rigorously. Less than three weeks after the first detected case in the country, New Zealand “shut its borders to outside travelers, and a week later had not only shut down non-essential businesses but went even further, instituting a ‘level 4 lockdown’ which meant that people could only interact with people within their home in an attempt to ‘eliminate’ the virus altogether (accompanied by emergency text messages that plainly explained what was expected of individuals).” New Zealand’s Prime Minister, Jacinda Ardern, put out Facebook live videos explaining the government guidelines and reinforcing the importance of strict adherence to them.
After more than 100 days during which the country was completely COVID-free, New Zealand has recently seen a small outbreak of still unexplained origin, but has rapidly instituted testing, contact tracing and isolation to contain the outbreak. Despite Donald Trump’s recent attempt to deflect attention from the miserable performance of his own U.S. government by labeling this small outbreak as a “big surge” in New Zealand, Ardern’s country has managed to keep its cumulative confirmed cases, as of August 25, to 1339 and COVID-19 deaths to 22 (or 4.6 per million inhabitants), compared to more than 5.7 million cases and more than 177,000 deaths in the U.S. by that date.
The success of lockdowns depends on three elements: (1) consistent, non-politicized, messaging from national governments about the importance of strict adherence; (2) ample government economic stimulus and guarantees to tide businesses and the population through hard financial times; and (3) adherence to scientifically driven metrics (e.g., for transmissivity measures or positivity rates from widespread testing) for a decision to lift the lockdown fully, or even partially. For example, the Australian national government, despite an earlier track record of clashes with scientists, established a national COVID cabinet comprising federal and state leaders from across the political spectrum to coordinate scientifically supported responses and consistent messaging. They provided an economic stimulus corresponding to more than 10% of the country’s Gross Domestic Product (GDP) to support wage subsidies, doubled unemployment benefits, and offered free childcare for all. Despite initial success in controlling the pandemic, a recent surge has brought the COVID-19 death rate in Australia to 18.5 per million inhabitants, still a factor of 30 below the U.S. per capita death rate.
In the U.S. meanwhile, the federal government – after disastrously failing to set up early testing or contact tracing – has refused to establish a national policy, has seen political leaders systematically undercut messaging from medical professionals, and has been inconsistent and partisan even in recommending the adoption of social distancing and mask-wearing measures. Control of a virus that is easily transported across borders has been left to individual states, with results that varied widely with the party in power in those states. The Centers for Disease Control recommended sensible metrics and guidelines for state reopening of their economies, but very few states chose to follow those guidelines, with the vast majority reopening before community spread was under adequate control. Incoherent messaging, combined with partisan support among politicians and members of the public for ignoring common sense mitigation strategies in the name of “individual liberty,” have resulted in the failure to control the pandemic, and in the ongoing rapid increase in cumulative COVID-19 deaths seen in Fig. 4.1.
While the U.S. Congress continues to be mired in partisan debate over the need and magnitude for a second short-term economic stimulus response to the ongoing pandemic, other countries have adopted a longer-term view. New Zealand, for example, has established a new fund equivalent to 17% of GDP “to keep jobs and reduce the unemployment rate over the next two years.” This follows a decision by the Prime Minister and her ministers to take a 20% cut to their own salaries, and to promise that no citizen would lose their residence if they lost work during the economic shutdowns in the country. Multiple government stimulus packages in Singapore have committed 20% of that country’s GDP to keep its economy afloat during the pandemic. The countries that have controlled the pandemic well understood that their economies can fully recover only after the virus has been reduced to levels that no longer threaten exponential community spread, so that the public feels safe in participating in the economy.
One of the small number of countries with a per capita COVID-19 death rate even higher than that in the U.S. is Sweden, whose government decided to avoid extensive shutdowns and government mandates, in hopes that enough Swedes would get infected to attain herd immunity to the virus. The goal of herd immunity is, at best, an elusive one for a virus where infection appears to give only partial, short-term immunity to those infected, and the virus mutates rapidly enough to make people susceptible to reinfection. Thus, the jury remains out concerning the wisdom of Sweden’s approach, in light of its terrible toll to date. Nonetheless, Donald Trump has now taken on a new coronavirus advisor who urges him to base U.S. strategy on attaining herd immunity despite the enormous (more than 2 million) continuing death toll such attainment would necessarily involve, if attainment is even possible. Trump may thus choose to emulate not the best practices from many other countries, but rather one of the very few countries with a higher COVID-19 death rate than the U.S.
In countries with clear national policies driven by a consensus among science and health professionals, and uncorrupted by partisan wrangling, governments have been rewarded with high approval rates for their handling of the coronavirus pandemic. For example, 93% of Australians and 84% of New Zealanders approve of the way their governments have handled the pandemic, despite the resulting economic hardships. In South Korea, President Moon’s overall approval rose to 71% as a show of public support for his handling of the outbreak. Meanwhile, in the most recent mid-August survey, only 23% of Americans strongly or somewhat approve of the federal government’s handling of COVID-19, while 57% strongly or somewhat disapprove. The view of the U.S. response from outside the politically polarized American populace is even more damning, as illustrated in the Australian survey results in Fig. 4.2.

Trump complains because many European countries are managing to reopen schools for in-person education this Fall, while most communities in the U.S. are ignoring his entreaties to do so. Denmark, for example, was the first country to reopen schools, which they could do safely because they managed the pandemic well and aggressively from the start, they instituted careful policies for limiting student groups, and they continue to test inhabitants at a per capita rate twice that of the U.S., while experiencing positivity rates nearly 100 times lower than those in the U.S. Non-partisan, science-based policy has provided global best practices in dealing with the pandemic, but the U.S. federal government continues to resist learning from those best practices.
False Claim #5: “Advice from top U.S. scientists about the coronavirus has consistently been wrong”
In previous blog posts, we have written about a 50-year right-wing effort to dispute and discredit the scientific consensus on many issues, particularly those where government regulation policies are supported by mainstream science. We have reviewed efforts in science denial as played out in skirmishes over smoking, insecticides such as DDT, and the ozone layer.
During the coronavirus pandemic, the Trump Administration has frequently found itself contradicting scientific advice on the best ways to prevent and treat the SARS CoV-2 virus. We have detailed how we began with the narrative “It’s completely under control.” This was followed by the narrative “It’s serious, but we’re doing a great job,” which was followed by “These are just recommendations, and we need to re-open the economy right away!”
Probably the most visible public-health member of the Coronavirus Task Force was Dr. Anthony Fauci, a world authority on infectious disease since the first days of HIV/AIDS. In contrast to other medical authorities who were less inclined to say anything that might contradict Trump, Fauci was relatively outspoken. When Trump insisted that the epidemic would “disappear, like magic,” Fauci said that he could guarantee it would still be around in the fall. When Trump urged states to re-open their economies before they met the criteria set out by the CDC, Fauci recommended caution and warned of new “spikes” in cases if states opened too soon.
Fox News commentators go to great lengths to validate whatever Trump asserts, and to attack anyone who seems to oppose Trump’s agenda. So Anthony Fauci was a natural target of Fox News commentators, as discussed in False Claim #2 in part I. However, other public-health agencies have also come in for their share of criticism. Right-wing critics have also focused on projections of COVID cases and deaths from groups such as the Institute of Health Metrics and Evaluation (IHME) at the University of Washington, and the Coronavirus Resource Center at Johns Hopkins University (JHU).
Following are two of the most common complaints about scientific advice during the pandemic.
- Scientists Frequently Contradict Themselves:
The scientific method works by forming a hypothesis and then testing it against data. If the hypothesis does not fit the data, it is modified or discarded and a new hypothesis is advanced. Although the coronavirus shares some properties with the common flu, there are also many novel qualities of the COVID-19 pandemic. For example, the SARS-CoV-2 virus is considerably more infectious than the flu and it is also many times more deadly. In addition, the large number of asymptomatic cases of COVID that are nonetheless capable of transmitting the virus to others make it much more difficult to control. It is only relatively recently that we have understood the role of airborne aerosols in spreading the disease. The number of cases and deaths that we can expect from this pandemic are predicted with the help of models. However, the models depend on a number of factors: how the disease is transmitted; the number of “super-spreader” episodes; contributing health factors in those who contract the disease; and the behavior of the public regarding wearing of masks and social-distancing. As those factors change and as scientists gather more data about the disease, their models should become progressively more reliable and the uncertainties associated with model predictions should decrease.
In the case of Anthony Fauci, we know of two instances where he reversed himself. The first was whether people should wear masks. At the beginning of the pandemic in the U.S., Fauci was worried about what seemed to be a “run” on personal protective equipment (PPE), including masks, for front-line medical professionals. At that time, Fauci recommended against wearing of masks; however, as the hoarding of PPE abated, and scientists realized that masks could play a significant role in reducing transmission of the virus, Fauci reversed his recommendation. A second instance was whether to restrict travel from China at the beginning of the pandemic. Fauci initially recommended against blocking travel from China; however, by the time President Trump announced a ban on travel from China (and it was a ‘leaky’ ban, with some 40,000 Chinese traveling to the U.S. over the next few months), Fauci supported the travel ban.
In all other cases of which we are aware, Dr. Fauci’s statements have evolved along with our knowledge of the COVID-19 pandemic. His recommendations for preventive measures to slow the spread of the virus agree with the best current scientific knowledge available on this health crisis, and he concentrates on telling the public what is likely to happen if they don’t follow guidelines issued by health professionals. His persistent warnings about the dangers of reopening economies or schools too soon, and of large gatherings without social distancing, have been borne out by the continuing spread of the virus in the U.S., after it had been successfully contained in many other industrialized countries. Furthermore, Fauci’s comments have been entirely consistent with the consensus of the worldwide community of infectious disease experts, as represented, for example, by WHO Director-General Dr. Tedros Adhanom Ghebreyesus, Dean Ashish Jha of the Brown University School of Public Health, and Dr. Thomas M. File, Jr., President of the Infectious Disease Society of America.
In contrast to Fauci’s advice, Donald Trump has encouraged people to flaunt the mask-wearing protocols, so much so that wearing a mask has become a politically-charged decision. Trump also incited states to re-open economically before they satisfied the CDC guidelines for re-opening; this was clearly based on the timetable before the federal elections in November. And Trump continues to hype the anti-malaria drug hydroxychloroquine (HCQ) as a treatment or preventative for the virus.
Some of the more bizarre comments about the coronavirus have come from White House economic advisor Peter Navarro. First, Navarro claimed or strongly hinted that the coronavirus was deliberately released by the Chinese to target Donald Trump and the American economy. “We were cruising along until the Chinese Communist Party basically hit us with that deadly virus, that weaponized virus,” Navarro told Fox News. “And I don’t think it’s any coincidence that the first year that China had a down economy was the same year now that they’re coming after us in all sorts of ways.” Navarro then told CNN reporter Erin Burnett, “We have the Chinese communists effectively sending a virus over here, whether it was done by accident or on purpose, I don’t know, but they send it over here and they basically kill over 150,000 Americans, cause trillions of dollars of damage.”
In a July 2020 op-ed column in USA Today, Navarro said that “Anthony Fauci has been wrong on everything I’ve interacted with him on … When Fauci was telling the White House Coronavirus Task Force that there was only anecdotal evidence in support of hydroxychloroquine to fight the virus, I confronted him with scientific studies providing evidence of safety and efficacy.” When confronted by Erin Burnett about this comment, Navarro replied “There is just disagreements, on things like, for example, the hydroxychloroquine, [Fauci] has a strong point of view, there are as many doctors on the other side.” “But there aren’t,” Burnett shot back. “Yeah there are,” Navarro said.
On both points, Navarro is completely wrong. As we have mentioned, scientists who have examined the structure of the SARS-CoV-2 virus insist that there is no sign that it was synthetic or that it did not originate naturally. Navarro’s dispute with Fauci over the effectiveness of hydroxychloroquine to treat COVID-19 again reveals Navarro’s ignorance of science. When pressed by Trump and his supporters over this drug to treat the coronavirus, Fauci merely said that these early claims were “anecdotal,” that is, that they were not the result of large-scale, statistically significant, blinded trials but were claims made on the basis of small event samples. In this regard Fauci was 100% correct: the early claims were anecdotal. The only large-scale, randomized trials with control groups that have been completed to date show that HCQ is not only ineffective in treating or preventing COVID-19, but that the side effects of this drug could be serious for some coronavirus patients. However, even if HCQ turned out to be an effective treatment for the pandemic, Fauci’s remarks would still have been correct: the early promising claims were in fact anecdotal. Navarro’s claim that “there are as many doctors on the other side” (i.e., that claim the drug is effective) is also patently false. This is typical of “scientific” comments made by the Trump White House during the pandemic. This is discussed in more detail under False Claim #9 in Part III of this post.
2. Scientific Predictions Change Wildly Over Time
By now there are a number of models that attempt to project the number of COVID cases and deaths. For example, MIT has produced an epidemiological model that forecasts cases, hospitalizations, and deaths. This is a so-called SEIR model (susceptible-exposed-infected-recovered). There is also a model from Los Alamos that uses as input the number of cases and deaths in a population in the previous time step, tries to determine the number of infected and susceptible individuals and multiplies those by a “dynamic growth parameter.” The projections are then compared with data and updated.
However, the most-cited projections of cases, hospitalizations and deaths are from the Institute for Health Metrics and Evaluation (IHME) at the University of Washington. Numbers from IHME are frequently quoted in news reports of the spread of the COVID pandemic, and are also projections that are widely used by the Trump White House. Non-scientific commentators frequently complain about the tremendous variability of forecasts from IHME: for example, in late March the best estimate of total number of American deaths from COVID was about 161,000; while in early April the “best estimate” was just over 60,000 deaths.
Citing the variation in these predictions, some right-wing commentators have called for congressional hearings into not only the infectious-disease models, but all modeling. Texas Senator John Cornyn tweeted “After #COVID-19 passes, can we have a good-faith about the uses and abuses of ‘modeling’ to predict the future. Everything from public health, to economic, to climate predictions. It isn’t the scientific method, folks.”
Actually, it is the scientific method. In situations that are too complicated to use first-principles scientific theories, we rely on models for guidance. First-generation models are often quite simple: they can give only general guidance on how the systems evolve, but not quantitative predictions. As time goes by, more and more forces are added, and model parameters are adjusted to agree with past observations. The success of the models is then judged by their ability to predict the outcomes of future events.
There is a clear review of models of pandemics on FiveThirtyEight.com, titled “Why It’s So Freaking Hard to Make a Good COVID-19 Model.” That article points out that determination of, say, the fatality rate from a disease is in principle quite easy. The number of fatalities (Ndead) is given by:
Ndead = Nsusc x Ninf x Rfat.
That is, the # of fatalities is given by the susceptible population (Nsusc ) times the rate of infection (Ninf) times the fatality rate of infected individuals (Rfat). However, each of these is itself dependent on many factors, several of which may be poorly known. For example, for COVID the fatality rate is known to change dramatically depending on the age, gender, race or even the blood type of the infected individual. In addition to that, the fatality rate also depends on co-morbidities, such as diabetes, hypertension or obesity. So there can be dramatic differences in the fatality rate between different countries, but even in different areas – we would expect the fatality rate to differ, perhaps dramatically, between areas such as metropolitan New York City and, say, Wyoming. Furthermore, the infection rate is sensitive to federal, state and local government policies and to public behavior, all of which are changeable and hard to predict. The 538.com article describes the eventual inputs and uncertainties in an epidemiological model as given in Figure 5.1. This shows a typical chart giving a set of elements that would enter into an epidemiological model to calculate the expected number of deaths in a pandemic. Yellow boxes denote factors that enter into the susceptibility rate; pink boxes are factors that enter into the infection rate; and blue boxes are factors that enter into the fatality rate. The takeaway is that these models contain very many factors.
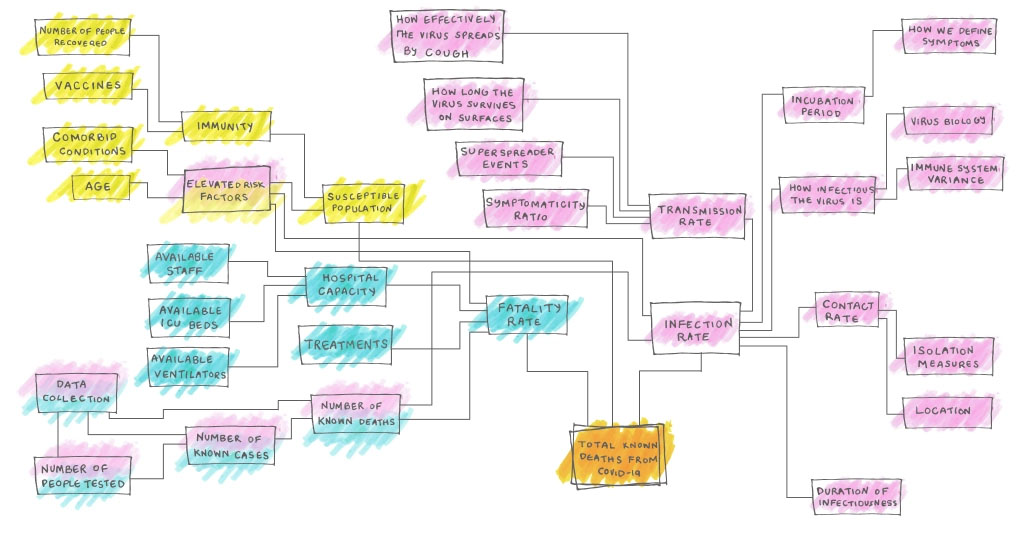
Figure 5.1. Ingredients of an epidemiological model of the number of deaths in a pandemic. Yellow boxes: factors entering into susceptibility rate; pink boxes; factors entering into the infection rate; blue boxes: factors entering into the fatality rate.
Political responses to IHME data tend to focus on the extent to which the IHME predictions agree with one’s political stance. However, epidemiologists and statisticians also are critical of the IHME approach, and we will summarize those criticisms here. First, unlike several other models, the IHME model is not guided by epidemiological knowledge about the susceptible population and the infection rate – it is a purely statistical estimate of the process. The IHME model starts with statistical fits to the course of the COVID infection in China and Italy. It then regularly updates those fits to account for the progress of the disease in the U.S.
One of the aspects of the IHME model that make it useful to government officials is that it was among the first to provide projections for individual states or counties; IHME published those projections before other models. In addition, the IHME projections included projections of hospitalization rates for individual locations, which helped greatly in planning for health emergencies. Finally, the IHME model was among the first to model the effects of social-distancing methods in slowing the spread of the disease.
However, there was one serious flaw in the early IHME models, and that is they assumed the course of the disease would follow the Chinese or Italian experience: once the number of cases and deaths reached a peak, the IHME model initially assumed they would rapidly and monotonically decline. This meant that, paradoxically, while the IHME projections might give a reasonable estimate of the uncertainty in a few days, as one projected further into the future, not only would the number of predicted COVID cases decline sharply, the claimed uncertainty would also decrease. Figure 5.2 shows the IHME predictions for COVID cases in the state of California, beginning on May 1. The projected uncertainty on May 3 is between 5 and 103 cases. However, by May 20, the IHME model was predicting zero COVID cases, with an uncertainty of zero! It makes no sense that a statistical model should have less and less uncertainty with increasing time, unless one is absolutely certain about how the number of COVID cases will change in the future.
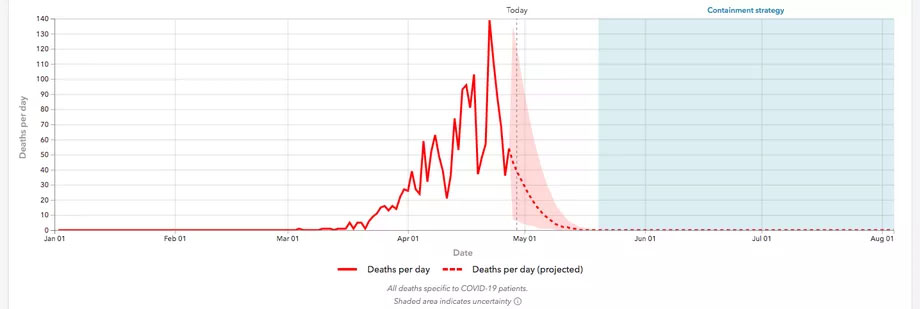
Figure 5.2. IHME predictions of COVID cases for the state of California starting in the middle of May. Note that IHME predicted cases, and uncertainties, both go to zero by June.
To make sure she was not mistaken in her assessment of the IHME prediction, the author of a Vox article, Kelsey Piper, asked an IHME spokesperson about the COVID graph for California of Figure 5.2; she was told, “Based on the graph, in certain states, yes — in California, May 17, zero. The virus is not circulating anymore; you would expect it to go to zero.”
Since the IHME model is constantly being updated, we assume that this serious flaw has now been removed from the program (otherwise there is no way they could reproduce the second peak in COVID cases over much of the country). But this flaw had dire consequences for the U.S. effort against COVID. In April, the Director of the IHME Christopher Murray was supremely confident that their prediction of a sharp decline in COVID cases would be borne out. “We believe in fitting models to data, and not making an assumption and then saying how my assumption would play out in a hypothetical world,” said Murray.
Many scientists were not convinced that the IHME projections of very rapid decline in COVID cases were accurate. Yale School of Medicine epidemiologist Gregg Gonsalves stated, “I fear the White House is looking for data that tells them a story they want to hear, and so they look to the model with the lowest projection of death.” In retrospect, this seems to be just what happened. In April, the Trump Administration latched on the fact that IHME projections showed the number of COVID cases going rapidly to zero. “It looks like we’ll be at about a 60,000 mark, which is 40,000 less than the lowest number thought of,” said Trump on April 19, referring to the IHME projection of total US COVID-19 deaths. Donald Trump’s oft-repeated insistence that the pandemic “will disappear – like magic!” might have been in part a result of reliance on the unphysical aspects of those earlier IHME projections.
False Claim #6: “The U.S. response to the coronavirus has been ‘The envy of the world,’ particularly with regard to our number of tests”
This is a self-serving claim made by Donald Trump, which is believed by almost no inhabitants of other countries (for example, see Fig. 4.2 above) and by a dwindling percentage of Americans. For example, only 15% of U.S. respondents to a mid-August Monmouth poll thought the U.S. was handling the pandemic better than other countries, in comparison with 52% who judged the U.S. response was worse than that in other countries. These views are reinforced by quantitative global metrics for judging the success of the response in different countries.

The U.S. has 4.3% of the world’s population, but nearly 25% of its confirmed COVID-19 cases. Its per capita COVID death rate is among the highest in the world, as illustrated in Fig. 6.1. When comparing per capita death rates for different countries, it is useful to introduce some consideration of the differing age distributions among inhabitants, since the mortality rate of the virus increases so rapidly among the elderly. Thus, in addition to plotting the total number of confirmed COVID deaths divided by the total population of each country in Fig. 6.1 (orange bars), we have also divided by the population aged 70 and above (blue bars, based on the percentage of elderly inhabitants indicated by 2015 global demographics). For example, Brazil has nearly the same overall death rate as the U.S., but Brazil’s population skews significantly younger, so its death rate among the elderly is quite a bit higher. The U.S. has the second highest death rate among the elderly, among the 15 industrialized nations included in Fig. 6.1. Take note of the logarithmic horizontal scale in Fig. 6.1, where each vertical line represents a factor of 10 change in the death rate. Thus, the elderly death rate in the U.S. is a factor of 100 higher than that in New Zealand or Japan, and a factor of nearly 10 higher than that in Germany.
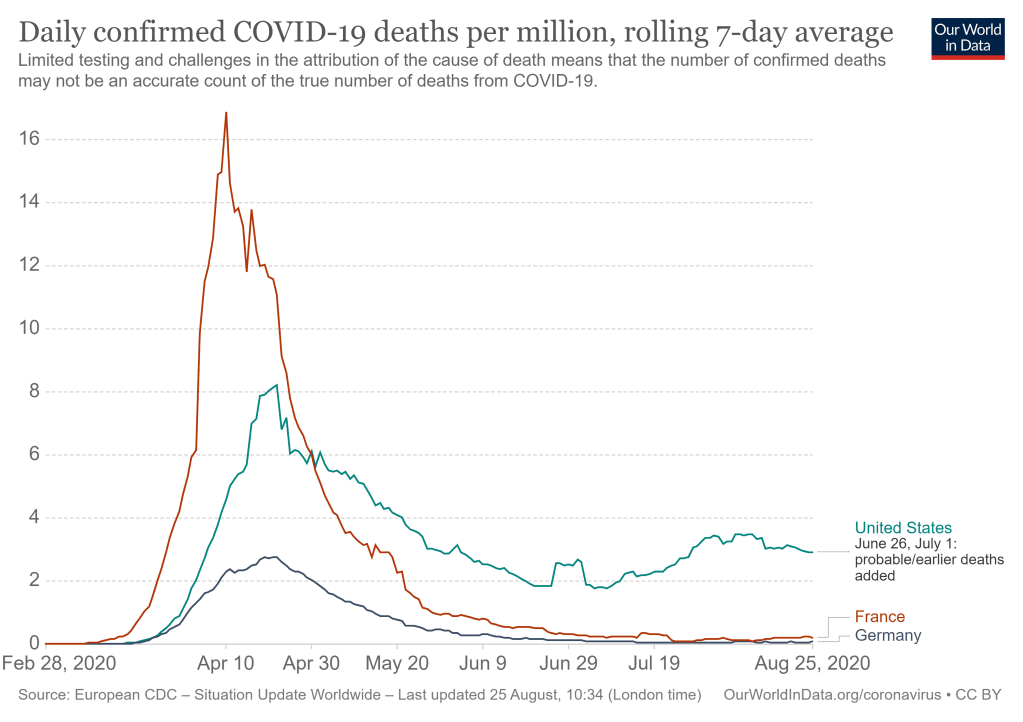
The nature of some U.S. failures compared to European practices is revealed by the comparison of daily COVID death trends in Fig. 6.2. France had significant exposure to the virus a couple of weeks before the U.S. and Germany, and saw the highest initial spike in mortalities, already at the start of April. The U.S. and Germany both had a little lag time to learn from the experiences in France, Spain and Italy. But Germany learned much more effectively, keeping its initial peak well below those in France and the U.S. The failure to adopt a national lockdown policy in the U.S. led to a range of policies and timelines among different states, with the effect of making the initial peak last longer. Germany and France waited until the pandemic was under reasonable control to begin reopening their economies, while many U.S. states reopened and allowed large public gatherings too soon, leading to the substantial second COVID death peak in the U.S. in July and August. A number of countries are now just beginning to see the onset of a second wave of the pandemic, as we will see below, while the U.S. is still dealing with strong, lingering effects of the first wave. And the U.S. still does not have a coherent national policy for dealing with the virus.
And what of the U.S. testing protocol, which Trump specifically calls the envy of the world? It is true that the U.S. has by now performed the largest absolute number of tests in the world. But the effectiveness of testing is dependent on several factors: how soon after the first cases widespread testing is initiated; what fraction of the population is being tested; what fraction of the tests return a positive result; how rapidly the test result is available; and how accurate the tests are (i.e., what are false positive and false negative rates?). The details of testing protocols are especially critical for COVID-19 because so much of the community spread of the virus appears to come from asymptomatic individuals. Unless these individuals are identified by widespread testing, and appropriately quarantined, community transmission of the virus may continue unabated.
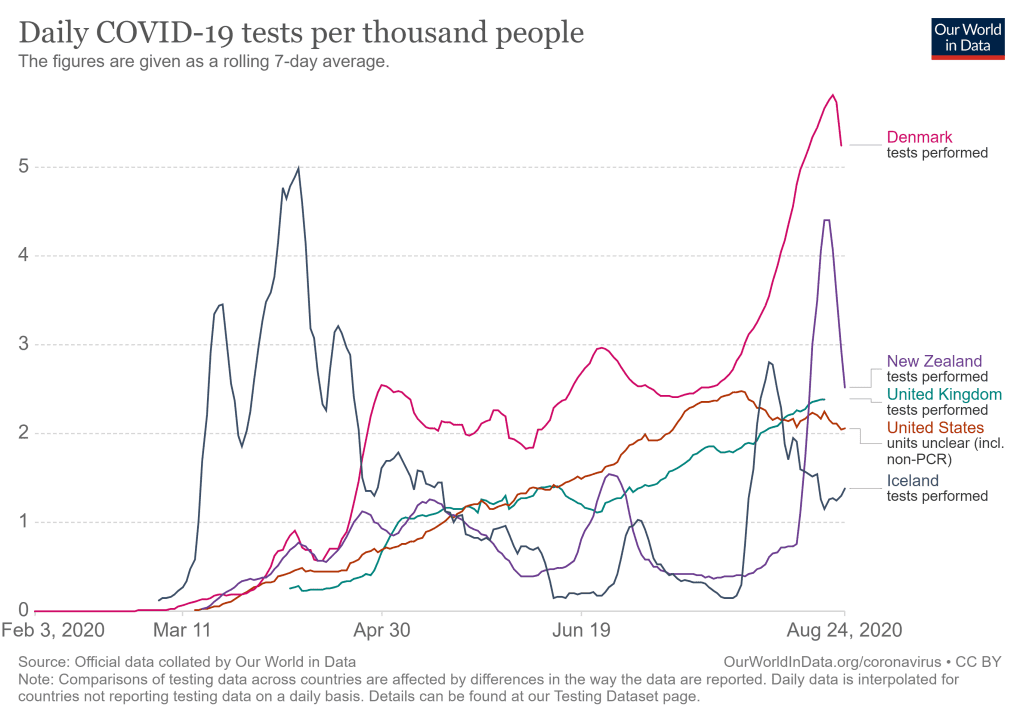
Figure 6.3 compares the U.S. per capita testing rates with those in several other industrialized countries. Several features of these curves are noteworthy. Iceland initiated rapid, aggressive, widespread testing in early March, just after the first cases were detected there. That allowed them to control the spread of the virus effectively from the start. In contrast, the U.S. ramped up its testing rate very gradually after a disastrously delayed start, thereby hampering efforts to control the pandemic in its early months. The U.S. finally reached a reasonable per capita testing rate in late July, but it is in no way extraordinary. Denmark, for example, has consistently tested a higher percentage of its population, despite having a testing positivity rate about two orders of magnitude lower than that in the U.S. A number of countries have ramped up testing rates rapidly in August, in anticipation of a second wave of the pandemic. New Zealand has launched an enormous, sharp increase in testing as a response to the still unexplained, but well contained, recent localized outbreak they have seen. During the same period in August, the U.S. testing rate has begun to decrease, even though the pandemic is far from contained.

Various features reduce the effectiveness of U.S. COVID-19 testing. As summarized in Fig. 6.4, the turnaround time to get results from tests is far too long. A July survey of more than 19,000 individuals across all 50 states plus the District of Columbia, carried out by a team from Harvard, Northeastern, Northwestern, and Rutgers Universities, has revealed that the mean waiting time nationally is 4.1 days, with only 37% of respondents getting their results within 2 days. Since most asymptomatic tested individuals do not self-quarantine while they await test results, many of them may infect others before learning that they have tested positive themselves. The problem is further exacerbated by a very unwise new August 24 guideline from the Centers for Disease Control, indicating that most asymptomatic individuals do not need to be tested at all. That guideline clearly reflects political pressure from the White House to keep the number of infected individuals from appearing too high during a Presidential election period, and it further complicates attempts to control the pandemic.
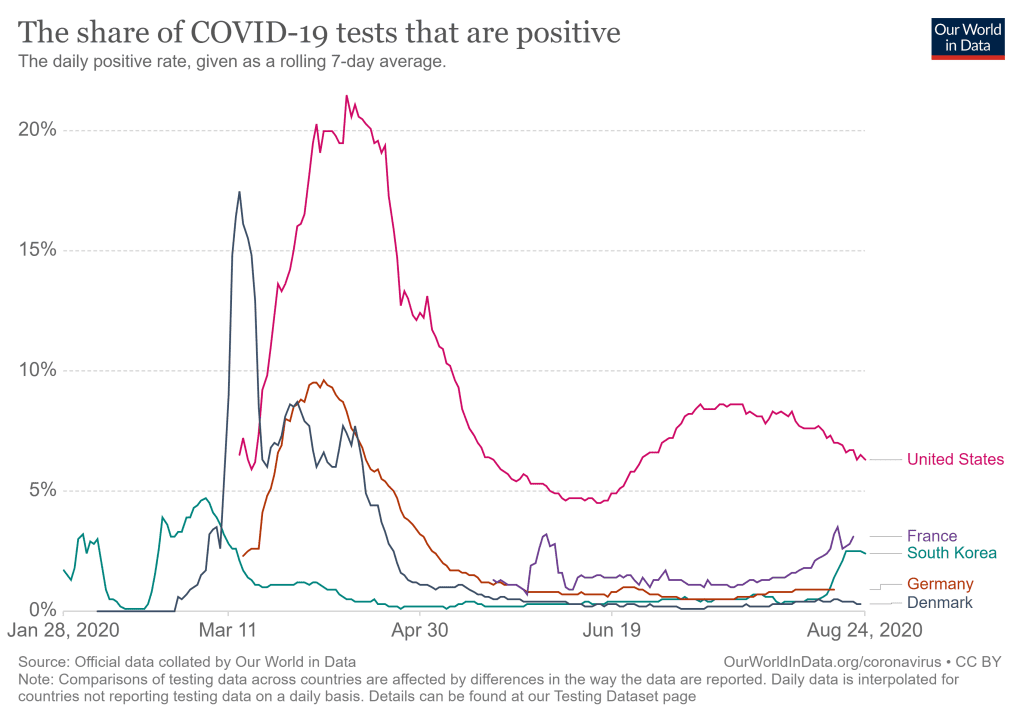
The trend in testing positivity rate in the U.S. is compared to that in several other countries in Fig. 6.5. The positivity rate is a leading indicator of COVID deaths to come; the U.S. curve in Fig. 6.5 looks similar to the U.S. death rate curve in Fig. 6.2, but with features shifted a few weeks earlier in time. While the national average positivity rate in the U.S. is now decreasing from its late July peak, it remains well above that in many other countries and well above the 5% level that the World Health Organization recommends as the threshold below which countries may begin phased re-openings of their economies. And in several states, the positivity rate is 2–4 times higher than the national average. The very recent upswings in positivity rate seen for France and South Korea in Fig. 6.5 may be harbingers of the anticipated second worldwide wave of the pandemic, which will further complicate the U.S. situation.
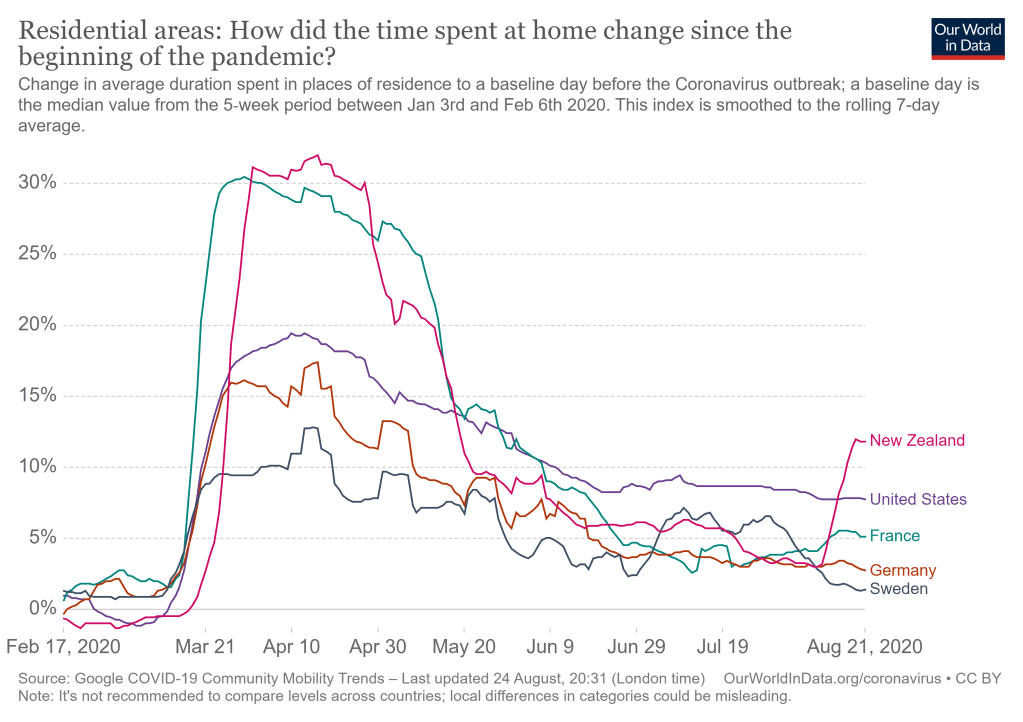
How do other features of the U.S. response to the pandemic compare to that in other countries? Donald Trump congratulates himself on the life-saving boldness of his decision to ban travelers from China, but the map in Fig. 6.6 reveals that the U.S. is one of many countries that have instituted comparable bans on travelers from high-risk regions (for most other countries, that category now includes the U.S.). A number of countries have gone further to implement total border closures. Figure 6.7 reveals that shelter-at-home policies adopted by some U.S. states were less effective, as a national average, than those policies in other countries, such as New Zealand and France. The map in Fig. 6.8 reveals that the U.S. carries out limited contact tracing, while a majority of countries around the globe do much more comprehensive contact tracing. There is thus nothing in the quantitative data, illustrated by Figs. 6.1- 6.8, to suggest that the U.S. coronavirus response is, or should be, the “envy of the world.” In fact, most of the world is simply baffled by the chaotic and ineffectual U.S. response and the continuing failure of the U.S. government to learn from its own past experiences or those of other countries.


False Claim #7: “The mitigations are worse than the disease”
People who object, for one reason or another, to adopting strategies that have been proven to mitigate community spread of COVID-19 promote specious theories about why those mitigations have worse impacts than the disease itself. Although this false claim is not unique to the U.S., many of the specious arguments have a quintessentially American flavor, highlighting alleged threats to “individual liberty” and the “American way of life.” Conspiracy theories have been especially prevalent with regard to effects of economic shutdowns, mask-wearing and vaccines.
As noted above under False Claim #4, many countries have successfully managed the first wave of the pandemic by mandating temporary (typically, 8—10 week) national shelter-at-home orders and shutdowns of non-essential businesses, supported by government economic stimulus packages and scientifically driven metrics for economic re-openings. However, the Trump administration appears to have made an assessment from the start that the President could successfully blame others for impacts of the disease, but he would shoulder the blame himself for losses of jobs and GDP. Thus, Trump himself echoed early claims that many more could die from suicide and despair during an economic shutdown than from COVID-19. This and similar attitudes led to the lack of a national U.S. mandate and to federal pressure on states to reopen their economies before community spread of the virus was under adequate control, producing the lingering COVID-19 death toll seen in Fig. 6.2.
The concern about deaths of despair, caused by unemployment, isolation and uncertainty about the future, is a real one. But in order to evaluate whether the mitigation is indeed worse than the disease, one needs some basis to estimate the losses. A reasonable attempt at such an estimate has been made by Stephen Petterson, John Westfall and Benjamin Miller of the Robert Graham Center and Well Being Trust. These authors have “used the quantifiable factors identified from prior economic downturns to estimate the number of additional deaths of despair due to COVID-19 impact on unemployment, isolation, and uncertainty.” As a baseline, they use pre-pandemic data compiled by the Centers for Disease Control, showing that in 2018 there were nearly 182,000 (or 55 per 100,000 inhabitants) deaths of despair – including suicides and alcohol- and drug-related deaths – in the U.S. as a whole, with considerable variation among age and ethnic groups, among states, and among different types of death. Previous analyses of correlations between the rates of such deaths of despair and unemployment rates suggest that each 1% increase in unemployment rate is accompanied by an increase in deaths of despair by something between 1% and 1.6%.

The authors’ models of COVID-19-induced unemployment rate are summarized in Fig. 7.1. All the models assume a peak national unemployment rate from state lockdowns of 15%, which is quite consistent with what has been observed. The assumed decay rates of the unemployment are tied to the decay observed in the U.S. following the 2008 Great Recession, when full employment occurred after a decade. The three models represented in Fig. 7.1 apply the same decay rate as for the Great Recession, twice that decay rate, or four times that decay rate. Even the most optimistic of these models is still considerably less optimistic than the recovery Trump has promised the country as part of his reelection campaign. Based on these three models and three different assumptions (1%, 1.3% and 1.6%) for the correlation between despair deaths and unemployment, the authors produce 9 sets of projections of possible incremental deaths of despair, as a function of year, resulting from the COVID pandemic-related unemployment. Those projections are summarized in the table in Fig. 7.2.

In the most optimistic of their 9 scenarios, Petterson, Westfall and Miller project an additional 28,000 deaths of despair spread over four years of recovery. The most pessimistic scenario would lead to 154,000 incremental deaths spread over 10 years of recovery. The broad range of possibilities reflects the large uncertainties in such an estimate. But all of the projections need to be compared with the more than 190,000 confirmed deaths from COVID-19 that have already occurred during the first six months of the pandemic spread in the U.S. Projected COVID-19 deaths now surpass 300,000, and that neglects the very real possibility of a second and third wave of the pandemic. Furthermore, the observed overall death rate in the U.S. in 2020, compared to the average of recent years, has been even higher, because it presumably includes additional disease-induced deaths caused by the unavailability of hospital beds during the peak of the pandemic in various states, and by increased public fears of going to the doctor or health care facilities. If there had been a nationally mandated lockdown in the U.S., accompanied by a much more rapid ramp-up in testing and contact tracing capacity, lifted only after COVID-19 test positivity rates reduced everywhere below 3%, then projected incremental deaths of despair would be somewhat larger than those in Fig. 7.2, but the cumulative number of COVID-19 deaths would have been greatly reduced. Contrary to False Claim #7, the tradeoff would have been well worth it, judging by the success other countries have had with a sensible lockdown policy.
Petterson, Westfall and Miller go even further, to break down their projections of deaths of despair by state, and even by county, but those projections have even greater uncertainty than the national ones in Fig. 7.2, so we do not present them here. These authors point out that their “report is not a call to suddenly reopen the country. Some might use this report to argue that this is why our economy needs to open up fast. But that’s NOT what we are saying.” Rather they propose a number of policy changes to address the mental health and addiction needs of the public, so as to minimize deaths of despair, while maintaining control of the pandemic. And they make note of the disparities in both COVID-19 and economic impacts across different communities: “Deaths of despair were a problem before COVID-19, just as health disparities were also a problem prior to COVID-19. What COVID-19 has done, is highlight yet again that the United States has not addressed underlying structural flaws in our systems. Issues of disparities are perpetuated by not addressing structural inequalities like employment, transportation, and income, making those at highest risk for losing their job or being exposed to COVID-19 communities who were already at a higher risk of a death of despair and now at even higher risk of dying to COVID-19.”
Other arguments that have been promulgated in right-wing circles in support of False Claim #7 focus more on the economic impacts of lockdowns – the cost-benefit analysis – than on deaths of despair. Apparently, the early laissez-faire approach taken to the pandemic by the White House was strongly influenced by a paper written in early March by libertarian legal scholar Richard Epstein, who told them what they wanted to hear. As we have previously covered on this site, Epstein made his own catastrophic underestimates of the pandemic health impacts and relied on them to argue that lockdowns being implemented worldwide were a gross over-reaction to a minor problem – no worse than the normal flu – and were likely to cause much more economic distress and strife than the virus itself. On March 16, he estimated that the U.S. would experience “about 500 deaths at the end” of the COVID epidemic. When that total was surpassed within the ensuing week, he explained on March 24 that he’d meant 5,000 deaths. As the death toll continued to rise exponentially, he arrogantly defended his expertise on the subject in a contentious March 30 interview with The New Yorker. He argued that public health measures against the disease “are done better at the level of plants, hotels, restaurants and schools than remotely by political leaders.” The striking differences in success between countries who took that approach and those that adopted clear national policies prove Epstein’s libertarian assumptions to be poppycock in this instance, as the U.S. death toll as of Sept. 8, 2020 passes 193,000 and is still rising rapidly.
Cost-benefit analyses to evaluate the wisdom of government-imposed lockdown policies to control the spread of COVID-19 are subject to enormous bias and uncertainty, and can therefore often be tuned to support one’s political preferences. Estimating the costs incurred by government action is not terribly difficult, at least after the fact, if one includes the known cost of economic stimulus packages and the recorded loss of GDP. However, there are the stickier issues of whether to include the costs of incremental deaths of despair and possible cost estimates incurred by social unrest resulting from prolonged lockdowns. In any case, one must subtract the costs of inaction, and these are much more difficult to estimate. How many additional deaths and hospitalizations would there be in the absence of government lockdown mandates? How many businesses would have to shut down, at least temporarily, because they became COVID hotspots? How much would consumer confidence and the economy suffer from a much wider and uncontrolled spread of the pandemic? And how much government economic stimulus would be needed in that case?
Estimates of benefits (or avoided costs) are much more subject to bias. Not only does one need model-dependent estimates of the additional lives that would have been lost, and the additional hospitalizations and long-term health issues avoided, if the lockdowns were not put into effect. In addition, one must decide the monetary worth of each extra lost life or lost year of productivity. Estimates of the monetary value to attach to a human life vary over a large range. Death compensation for military service is $100,000 per life, while the EPA during the Obama administration valued lives saved by regulations at about $9 million each. Health economists often use the Value of a Statistical Life (VSL), determined from the average incremental compensation paid to, and death risk assumed by, workers in high-risk jobs, converted to a value per year (VSLY) by dividing by the remaining years of life expectancy as a function of the worker’s age. But for some estimates they use instead a value of $100,000 — $150,000 per Quality-Adjusted Life Year (QALY), which permits reductions in effective life expectancy for the reduced quality of life associated with some chronic health problems. The quality of life reduction also often has a discount rate attached to it, so that later life years have a QALY contribution reduced by 3% or 7% per annum. The resulting variation in health economist estimates of the value of a statistical life for various age groups is indicated in Fig. 7.3.
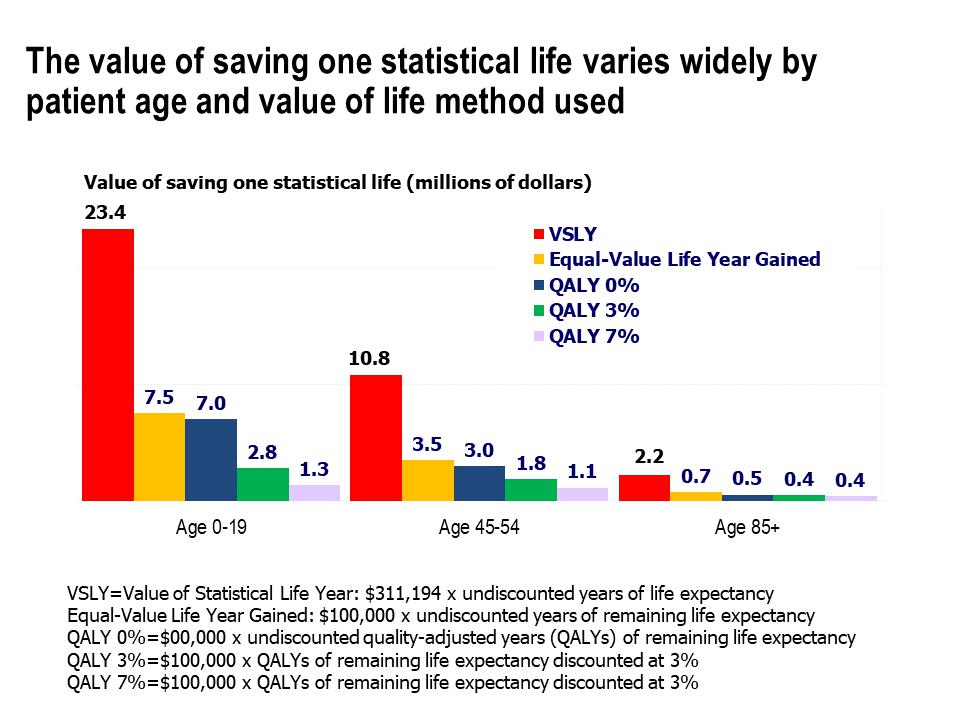
A recent paper from the Mercatus Center at George Mason University, reporting a cost-benefit analysis for COVID-19 suppression, uses a much more conservative estimate based on the benefit of avoided losses in work productivity, averaged over people of all age groups, and weighted by the COVID-19 mortality rate for each age group. The average benefit per life saved from death by COVID-19 then works out to $321,000, far below the other estimates in Fig. 7.3. Even that very conservative estimation of benefits in the Mercatus Center paper still leads, however, to a net estimated benefit of the various state suppression policies used to date to “flatten the curve” during the early stages of the COVID-19 outbreak in the U.S.
The costs and benefits of those state-imposed policies are evaluated “relative to a baseline in which only the infected and at-risk populations mitigate the spread of coronavirus,” i.e., without stay-at-home orders and restrictions imposed on non-essential business operations, schools and large public and private gatherings. The estimated benefits through August 4, summarized in the table in Fig. 7.4, include lives saved (based on model projections from the Imperial College of London and from the University of Washington Institute for Health Metrics and Evaluation), avoided hospitalizations, including Intensive Care Unit stays and ventilator needs, and avoided lost work from COVID-19 symptomatic infections and from long-term lung damage. The costs of state suppression policies relative to the individual mitigation baseline are estimated as equivalent to an 8.7% annualized loss in national GDP, scaled to the GDP contributions from individual states and the durations of their shutdown mandates.

The Mercatus Center analysis is well documented, but hardly definitive. Others have estimated much higher costs and much higher benefits. The bottom line is that there is such great uncertainty in any cost-benefit analysis that there can be no convincing validation of politically motivated claims that the economic costs of government-imposed mitigation outweigh the costs of an uncontrolled COVID-19 pandemic.
Six months into the spread of the pandemic in the U.S., some state and local governments – even after lifting restrictions on schools and non-essential businesses – have mandated, or at least strongly urged, the wearing of masks in public to mitigate the spread of virus-loaded aerosol droplets, especially when it is not possible to maintain distances of at least six feet from other people. It is important even for individuals who don’t feel sick to wear masks, because we know that much of COVID-19 transmission occurs from asymptomatic infected people. And we have by now seen numerous cases of large gatherings of unmasked people turn into COVID-19 “super-spreader” events.
But a vociferous minority of people, both in the U.S. and abroad, have objected strenuously to mask-wearing, claiming that it violates their personal freedom. Often they claim that it is their constitutionally mandated right to die of COVID-19 if they please. Such a claim overlooks the fact that, even if they are asymptomatic, they may be carriers and spreaders of the virus, and they are far more likely to transmit the disease to others if they don’t wear face masks. The U.S. Bill of Rights includes no constitutional guarantee of a right to infect others. The issue is one of protecting public health, and the federal, state and local governments have a responsibility to adopt policies that offer such protection.
In recognition of the weakness of their “personal freedom” claims, many “anti-maskers” have engaged in conspiracy theories based on false assertions that wearing masks causes more severe health problems than it prevents. The false assertions are epitomized by the evidence-free disinformation graphic in Fig. 7.5, which has been spread among anti-maskers. If any of these claims were true, one would expect the most vulnerable community to be hospital workers who wear surgical masks all day, year round, without experiencing any mask-induced health problems.
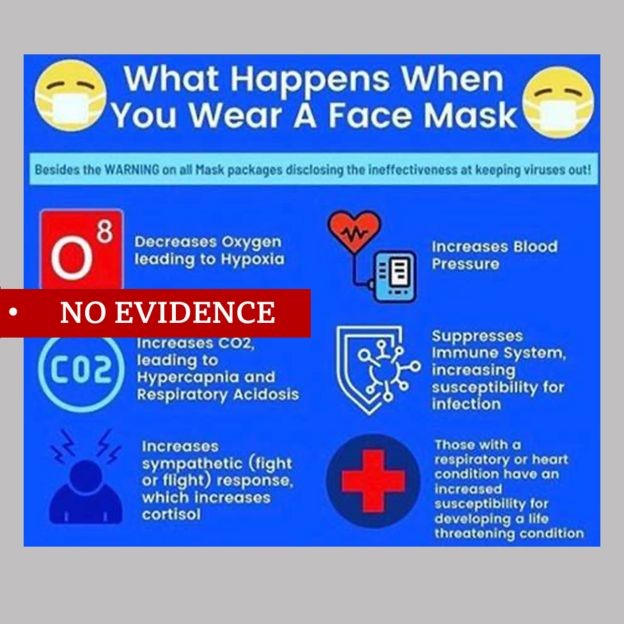
Face masks are designed to be breathed through, and there is absolutely no evidence to support the claim that wearing them reduces oxygen intake. Measurements of oxygen saturation levels with pulse oximeters show no change when the subject dons a surgical mask. Oxygen molecules are far, far tinier than the virus-containing droplets whose transmission the masks are designed to block. The same is true of carbon dioxide molecules, so claims that masks cause wearers to re-breathe their own exhaled CO2 and cause carbon dioxide toxicity are equally false. The American Lung Association warns that there is some evidence “that prolonged use of N-95 masks in patients with preexisting lung disease could cause some build-up of carbon dioxide levels in the body. People with preexisting lung problems should therefore discuss mask wearing concerns with their health care providers.” But in order for any significant reduction in oxygen intake or carbon dioxide release to occur in individuals without lung disease, they would have to be wearing airtight masks so heavy as to impede breathing all together, and those are not being sold to mitigate COVID-19 spread. Surgeons regularly wear much heavier-duty face coverings than most commercial face masks, and do so all day long, without any harm to their health.
There is similarly no evidence whatsoever to support the false assertion that face masks suppress human immune responses. Professor Keith Neal, an infectious disease expert, points out: “Masks may stop germs getting into your mouth or nose so your immune system doesn’t have to kick in, but this doesn’t mean it is being suppressed.”
Yet another claim made by anti-maskers is that face masks do not impede the spread of the virus. This is unfortunately true for some of the mesh and lace open-weave masks recently offered by some vendors to allow wearers to obey the letter, but not the spirit, of a mask mandate. But masks made from tight-knit materials, especially ones containing a filter pocket, do cut down enough droplet transmission to provide an effective mitigation against COVID-19 spread. A recent University of Arizona study has tested and rank-ordered face mask material from most to least effective. They found “that wearing a face covering slashed the risk of infection by 24% for a simple cotton covering and up to 99% for a professional, medical-grade filtration mask.” In particular, the name of N95 masks indicates that they are designed to block passage in or out of 95% of virus-containing droplets.
The anti-mask movement is largely politically motivated. Clear evidence of this is provided from comments Fox News personality Tucker Carlson has made to his considerable audience. On his March 30 evening TV hour, Carlson stated: “Of course, masks work. Everyone knows that. Dozens of research papers have proved it. In South Korea, Japan, Hong Kong, the rest of Asia — where coronavirus has been kept under control — masks were key.” Yet after it was made clear to him that many members of his conservative audience, and most importantly Donald Trump, did not like masks, he changed his tune on his July 7 show: “Many schools that do plan to reopen will do so under a series of restrictions that have no basis of any kind in science. It’s kind of a bizarre health theater. Students will be kept six feet apart, everyone will have to wear a mask, class sizes will be limited…” He was right the first time.
Yet another strain of the “mitigations worse than the disease” argument concerns vaccines. Even before we have an approved vaccine to mitigate (not absolutely prevent) COVID-19, anti-vaxxers have already started to roll out disinformation claiming that any such vaccine will be harmful. They have falsely claimed for years, without supporting evidence from legitimate scientific studies, that modern vaccines contain toxins and mercury compounds, that they cause autism, chronic fatigue syndrome, and other disorders. We have already debunked those claims in our blog series on Vaccinations. But in the context of COVID-19, the group has found a new champion in the person of Dr. Judy Mikovits, who was prominently featured in the viral Plandemic video.
Mikovits suggests that many animal viruses and retroviruses are transferred to humans through vaccines. She claims that once these contaminants are absorbed in the blood, they can remain dormant there for long periods of time, before eventually causing disease or weakening the human immune system. When an injected individual is later exposed to a disease, Mikovits claims they are likely to suffer a much more severe reaction than unvaccinated individuals with healthy immune systems. Her claims are strongly refuted by more trustworthy medical scientists, who find no evidence of viral material from chickens, mice or monkeys in the blood of vaccinated individuals.
In the context specifically of a potential COVID-19 vaccine, the anti-vaxxers’ favorite son Robert Kennedy, Jr. now appears to have joined forces with Judy Mikovits, QAnon supporters, the German conspiracy theory group Querdenken 711, and even Vladimir Putin in spreading misinformation to dissuade the public from participating in a vaccination program. The Russian government-funded TV channel RT has just published a video of part of Kennedy Jr.’s demagogic August 29 speech (see Fig. 7.6) to a large, raucous German crowd of Querdenken 711 supporters, in which he accused Bill Gates and Anthony Fauci of stoking fear about the COVID-19 pandemic in support of their plans for world domination. He described the pandemic as “a crisis of convenience for the elites who are dictating these policies” to control and surveil (via 5G technology and Bill Gates’ suite of satellites) the global public. In a statement he gave to the right-wing conspiracy podcast TruePundit, Kennedy Jr. accuses Fauci of having already “poisoned an entire generation of Americans” and seeking to poison more with a COVID vaccine. On the website of Kennedy Jr.’s organization Children’s Health Defense, he explicitly promotes the notion that COVID-19 health regulations support Bill Gates’ globalist agenda for mandatory vaccinations as part of a conspiracy led by Big Pharma, which will give Gates “dictatorial control of global health policy.”

The pandemic has now brought the anti-vaxxers from a fringe group largely populated by worried parents into the heart of the populist, right-wing conspiracy network that is threatening western democracies. This is a dangerous move for the vast majority of us who simply want to avoid contracting this highly transmissive and fairly deadly disease. We will discuss this in more detail in our review of False Claim #10 in part III.
